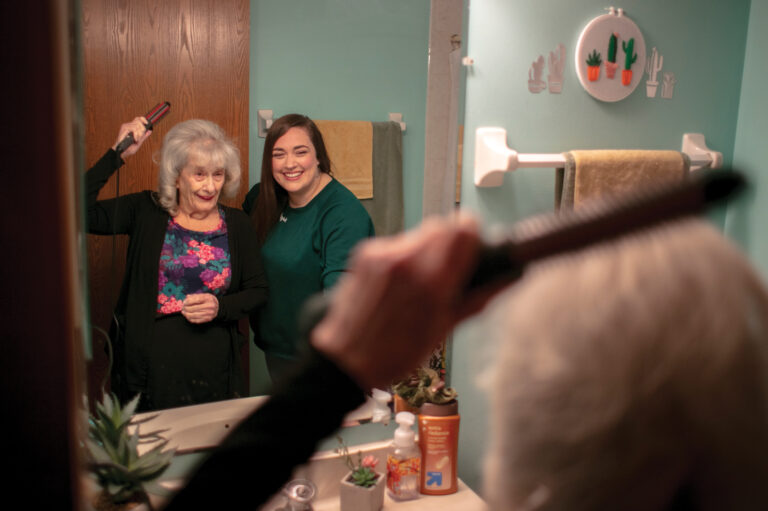Sarah is a longtime journalist, specializing in aging, parenting, caregiving, health, and business management topics.
Enhancing quality of life for people with dementia
Chicagoan Kris McCabe’s Instagram and TikTok accounts are peppered with sweet moments with her grandmother, Mary Padovani. Videos show the two singing a Patsy Cline song and sharing a hug as they swap, “I love yous.” In others, Padovani brushes McCabe’s hair, as she’s done for years.
These glimpses are part of a lifetime of memories made between the pair. But a closer look at McCabe’s accounts, titled Life with Grams, reveals a sad turn to the story. Padovani, 84, was diagnosed with Alzheimer’s disease more than five years ago, and she hasn’t called McCabe, 35, by name for about two.
But even as Padovani’s functioning has diminished, McCabe, who cares for her grandma full time from her home near Midway Airport in Chicago, has worked hard to embed meaning into her life. Padovani benefits — and McCabe does, too. Heartfelt moments in their videos attest to that.

“It’s all about the power of mindset and being mindful of your situation,” McCabe says. “I could sit here and cry every day. I could talk about how miserable it is. This morning, she didn’t want to change clothes, and she didn’t want to eat breakfast. Last night, she threw up. I’m dealing with a lot constantly. But I find those silver linings. I find those beautiful moments because that’s what life is focused on. You have to focus on the good stuff.”
People with dementia may not have the same abilities they once did, but it’s possible — and important for the individual and their caregivers — to make their remaining life the best it can be, experts say.
Exactly how to find that “good stuff” isn’t always clear or easy, especially as Alzheimer’s disease progresses. But the biggest mistake that caregivers make as they look for ways to engage with their loved ones is not understanding that their personality and preferences haven’t changed with their diagnosis, says Aishling Dalton Kelly, CEO of Aishling Care Academy and Aishling Companion Home Care in Orland Park.
Focusing on who that person has always been and adapting activities they’ve liked can make a difference in their remaining days, Kelly says. “Your inner soul and the essence of your being is still there. Sadly, we don’t focus on that. We focus on the disease and all the things they can’t do.”
Human desire for happiness
Like anybody, people with dementia need to stay engaged, connected, and active. Research shows the clear benefits. “It’s just a human desire,” says Susan Buehler, PhD, a clinical psychologist at Rush University Medical Center who works with people with dementia and has studied caregiver stress.
Contributing to family life and taking part in favorite activities, along with therapy and medication, are among the pastimes that can help people with dementia address depression.
Physical activity — even gentle exercise such as light housework — supports good health, from better sleep habits to improved muscle strength, for those with dementia, according to the National Institute on Aging.
Cooking and listening to music can bolster a person’s emotional state and reduce caregiver distress, according to a study published in the Journal of Alzheimer’s Disease.
Another study, published in Alzheimer’s Care Today, asked people with dementia and caregivers about quality of life. The two groups agreed on two important areas: positive mood and engagement in pleasant activities.
And it makes sense. “Research shows that participating in pleasant activities improves mood. Although it may seem challenging to engage in such activities when it comes to dementia, anything is possible with a little creativity,” Buehler says.
Staying engaged, connected
McCabe has gotten creative over the years as she cares for Padovani. The person her grandma has always been — a big personality who loves children and has a deep desire to be helpful — has guided her.
McCabe keeps those traits in mind as she plans Padovani’s days. She lets her wash the dishes, even if she’s not doing it quite right anymore. “If she doesn’t use soap, when she’s done with the dishes, I’ll use soap,” McCabe says.
They care for McCabe’s sister’s children — Padovani’s great-granddaughter and great-grandson — after school each day. Padovani enjoys following along with her great-granddaughter on workouts and playing basketball with her great-grandson.
And when Padovani says something that isn’t coherent, McCabe will respond to her in the very same way, mimicking her mood and even nonsensical words. “I repeat the gibberish just to try to get her to understand that I am listening, and I am here,” McCabe says.
Mindful of her own quality of life, McCabe attends therapy, takes breaks from her caregiving duties, and has found a community of support online and off to help her through trying experiences. “Every day is hard, and I always let people know that,” she says.
But engaging with her grandma — taking advantage of the moments they can connect — brings McCabe focus and deep joy, too.
“Whether this disease changes her or not, I know what her core is. I know her heart,” McCabe says. “And I’m very fortunate and very, very thankful that her core, the heart my grandma has, remains the same. Because the way she holds my hand, the way she looks at me, the way she hugs me, it tells me, whether she can say it or not, that she knows who I am and that she trusts and loves me. I really try to focus on that.”
And it gives her plenty of Life with Grams TikTok material, too.